Average Length of Stay (ALOS) is an essential metric your sales reps must understand when connecting with top referral sources in your market.
From cost-effectiveness to patient outcomes and regulatory compliance – ALOS can indicate the efficiency and quality of post-acute care services.
Throughout this blog, we will uncover:
- What average length of stay is in post-acute care
- What is the average length of stay in inpatient and skilled nursing settings, and how have these values changed since before COVID-19?
- How can home health and hospice agencies use those trends to articulate their value propositions to referral sources better?
By uncovering the factors driving these differences and the unique challenges faced by post-acute care organizations – you can gain valuable insights into how you can help your top referral sources effectively manage patient care and resources to enhance the quality of care.
What is Average Length of Stay?
According to the CDC – “average length of stay (ALOS) refers to the average number of days a patient stays at a facility.” Trella Health calculates the average length of stay by dividing the number of days under the care of a provider by the number of discharges.
So – why is average length of care important?
It’s vital for cost-effectiveness, resource allocation, and patient outcomes in post-acute care.
Inpatient and skilled nursing organizations aim to lower their ALOS to reduce expenses, optimize resource utilization, and minimize the risk of complications
Note: ALOS is a crucial metric for efficient, high-quality, patient-centered post-acute care services.
What is the average length of stay in inpatient and skilled nursing settings, and how have these values changed since before the COVID-19 pandemic?
Inpatient ALOS Trends
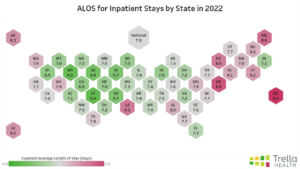
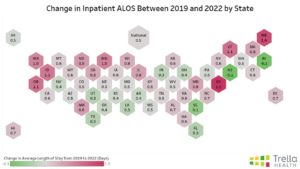
Overall, for inpatient care, the national ALOS for 2019 was 7.1, while in 2022, the national ALOS was 7.6 – therefore, the national ALOS increased by 0.5 days between the 2019 and 2022 calendar years.
States such as Delaware, Idaho, Maine, Oregon, and Vermont had the highest change in ALOS between 2019-2022, each increasing by 1.1 days or more.
Meanwhile, states such as Florida, Louisiana, New Jersey, Rhode Island, and South Carolina had the lowest change in ALOS between 2019-2022, increasing by 0.3 days or less. Notably, Rhode Island and New Jersey were the only states that saw a decrease in inpatient ALOS between 2019 and 2022.
Skilled Nursing Facilities (SNF) ALOS Trends
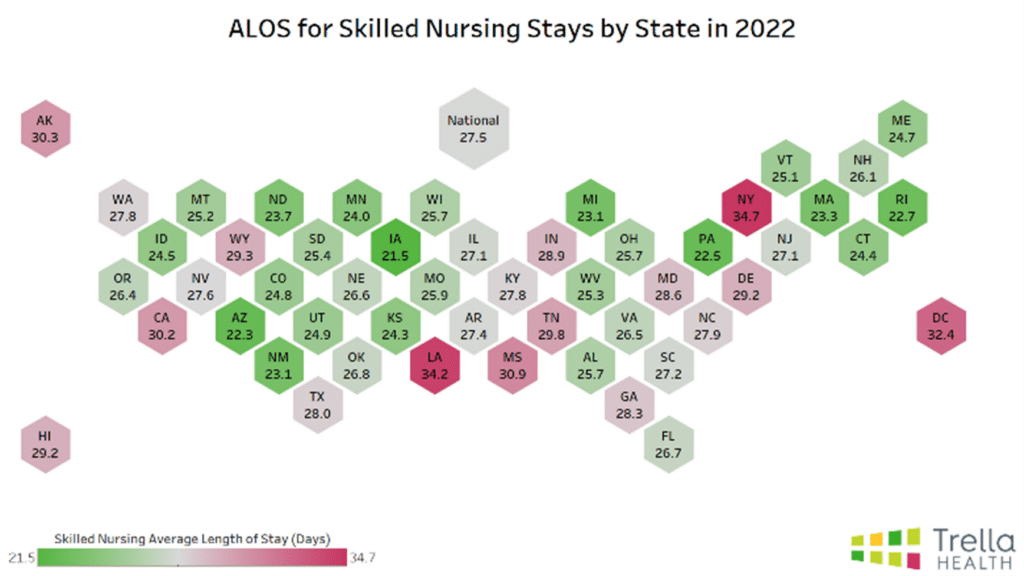
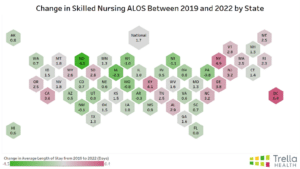
Overall, for skilled nursing facilities, the national ALOS for 2019 was 25.8, while in 2022, the national ALOS was 27.5 – therefore, the national ALOS increased by 1.7 days between the 2019 and 2022 calendar years.
States such as California, Delaware, Kentucky, New York, and Washington D.C. had the largest increase in ALOS between 2019-2022, increasing by 3.6 days or more.
In contrast, states such as North Dakota, Iowa, Michigan, Wisconsin, Pennsylvania, and Missouri had a decrease in skilled nursing ALOS by 0.8 days or more.
How can home health and hospice agencies utilize average length of stay trends to better articulate their value propositions to referral sources?
Home Health ALOS Trends
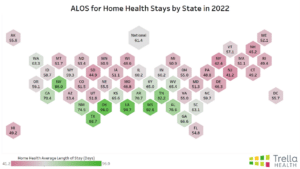
Home health agencies must effectively communicate how they can help decrease inpatient facilities’ ALOS without affecting outcomes.
It’s important to note that the ability to lower inpatient ALOS is essential to home health agencies’ core value proposition while directly impacting hospitals’ bottom line. Therefore, home health agencies that can illustrate their ability to decrease inpatient LOS are better positioned to build and maintain valuable FFS referral relationships.
This mutual understanding allows inpatient facilities to save costs by lowering inpatient length of stay while increasing valuable FFS admissions to home health agencies – while home health agencies can establish themselves as a top referral partner for Fee-for-Service (FFS) referrals and communicate their unique value in the market to top physicians.
Hospice ALOS Trends
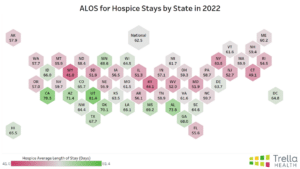
Similarly, hospice agencies should communicate with hospitals on how sending referrals earlier to hospice can help decrease their length of stay (LOS) for inpatient stays while ensuring patients will receive high-quality care at their agency.
Since hospice agencies want longer lengths of stay, earlier referrals from hospitals to hospice agencies are mutually beneficial in lowering inpatient LOS and readmissions while increasing hospice LOS.
Note: Trella Health excludes stays longer than two years in calculating hospice ALOS to avoid data skew caused by outliers. Understanding these variations helps post-acute organizations effectively manage patient care and resources in their line of business.
What’s next for average length of stay?
We’ve uncovered that ALOS is a crucial metric in post-acute care, influencing organizations’ cost-effectiveness, resource allocation, and patient outcomes.
Your sales reps must communicate to top referral sources how your organization can stand out regarding ALOS and help them reduce expenses, optimize resource utilization, and enhance patient care.
Want to learn more about how Trella Health’s data can help your organization stand out and help top referral sources with their ALOS?
Take the next step by exploring Trella Health’s innovative products.
Discover how our solutions empower healthcare organizations with valuable insights and data, allowing them to make informed decisions and enhance patient care.
To learn more, don’t hesitate to reach out to us for a personalized demo at https://www.trellahealth.com/demo
















