Ellen Knowles, Product Marketing Manager
As a results-driven marketing enthusiast with a focus on Healthcare IT and SaaS-based business, Ellen helps achieve strategic goals for market growth, product adoption, and customer success as a Product Marketing Manager at Trella Health. Ellen spent time at Georgia Military College before moving to Atlanta to start her career in sales, but quickly found her passion in marketing and dedicated the last four+ years to growing health IT brands and business in the hospital and ambulatory. At Trella Health, she's able to continue her passion for innovation and meaningful results.FY 2022 Final Rule: What the New Hospice Quality Measures Mean for You
By Ellen Knowles | October 22, 2021
After announcing the FY 2022 Hospice Final Rule, CMS hosted an online forum to provide details and need-to-know info on the Hospice Quality Reporting Program (HQRP) – specifically addressing the new Hospice Quality Measure Specifications User’s Manual v1.00 (QM User Manual) and the forthcoming changes to two of the program’s four quality metrics (QMs).
To help hospice providers prepare for the coming year, we’ve put together a few key highlights from the forum, including important dates and details to keep in mind as you prepare your 2022 strategy.
Key Dates and Deadlines for FY 2022
According to CMS, “providers have 4.5 months following the end of each calendar year (CY) quarter to review and correct their [Hospice Item Set (HIS)] records with target dates … in that quarter for public reporting.1 If you miss this deadline to correct your records, your existing HIS data will be “permanently frozen for the purposes of public reporting. Updates made after the correction deadline will not appear in any subsequent Care Compare refresh.”1 However, be aware that you’re HIS-Admission and HIS-Discharge records may not have the same data correction deadlines, as these deadlines are set at the HIS record level.
To allow for the disruption created by the COVID-19 public health emergency (PHE) in 2020, HQRP data submission deadlines were temporarily exempted for affected quarters. That exemption will soon come to an end, and public reporting will begin again with the February 2022 records refresh. Per CMS, upcoming HIS record data correction deadlines for public reporting are:
- Q3 2021: February 15, 2022
- Q4 2021: May 16, 2022
- Q1 2022: August 15, 2022
- Q2 2022: November 15, 20221
FY 2022 Hospice Final Rule: Updates as of August 2021
In August 2021, CMS hosted a training webinar on what hospices need to know about the FY 2022 Hospice Final Rule. The purpose of this webinar, according to CMS, was to “educate providers about the changes in the [HQRP] as a result of the Hospice Final Rule. In addition to a brief summary of the history of HQRP and an overview of CMS’ annual rulemaking process, the webinar covered:
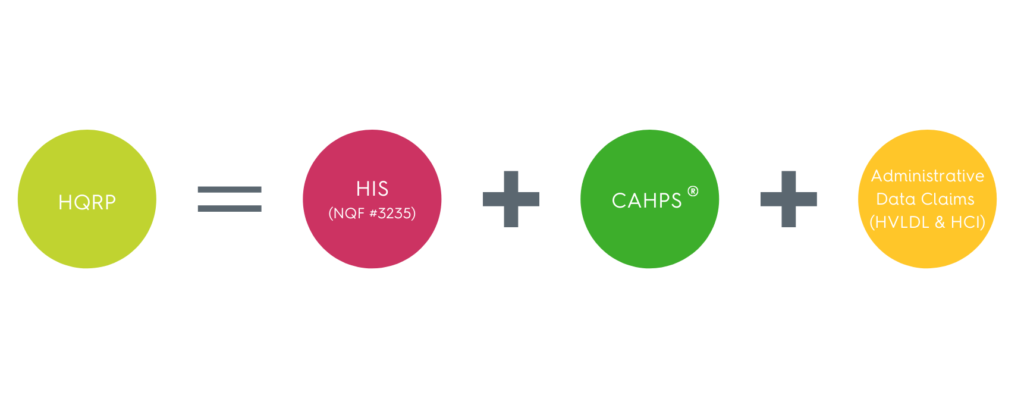
- Sources of data used to fulfill HQRP requirements:
- HIS data collection and submission.
- CAHPS® Hospice Survey submission.
- Administrative data (Medicare claims).2
- Changes to the HQRP for FY 2022:
- The HQRP now consists of four Quality Measures (QMs).
- The seven individual HIS process measures have been removed.
- Claims-based measures have been added:
- Hospice Visits in the Last Days of Life (HVLDL).
- Hospice Care Index (HCI).2
FY 2022 Hospice Quality Measures: October 2021 Webinar Highlights
Building upon the topics covered in CMS’ August webinar, the October forum gave an overview of the new QM User Manual v1.00. This manual, which is available at CMS’ website in the downloads section at the bottom of the page, does not include a table of highlighted changes from the previous version. CMS’ Cindy Massuda explained in the forum that this is because the current manual is not an updated version of the old manual but rather an entirely new text. In it, hospices can find information on:
- The Hospice and Palliative Care Composite Process measure (based on Hospice Item Set (HIS) data)
- The Hospice Visits in the Last Days of Life (HVLDL) measure (based on 8 quarters of Medicare hospice claims data, replaces the Hospice Visits When Death is Imminent measure)
- The Hospice Care Index (HCI) measure (based on 8 quarters of Medicare hospice claims data)
- Specifications for each QM3
Beyond reviewing the QM Manual, the forum touched on what hospices need to know about changes coming to the HCI and HVLDL measures. No updates were made to the other two measures, and hospices should continue reporting on them as before.
Both HVLDL and HCI are claims-based measures. HVLDL is measured based on the number of qualified hospice staff visits (e.g., RN or medical social worker) within two of the last three days of life. HCI is a composite measure based on 10 indicators, each of which is worth one point. Thus, HCI scores will range from 0 for a hospice that meets none of the indicators to a perfect 10 for a hospice that meets all indicators. These indicators are:
- CHC/GIP provided
- Gaps in skilled nursing visits
- Early live discharges
- Late live discharges
- Burdensome transitions (Type 1)
- Burdensome Transitions (Type 2)
- Per-beneficiary Medicare spending
- Nurse care minutes per routine home care days
- Skilled nursing minutes on weekends
- Visits near death3
Both of these claims-based QMs will be based on an eight-quarter reporting period. Taking into account the exempt quarters due to COVID-19, the first reporting period for the FY 2022 Hospice Final Rule will be represented by:
- Q2, Q3, Q4 2019
- Q3, Q4 2020
- Q1, Q2, Q3 2021
These measures will be reported publicly no earlier than May 2022, and hospices will have access to confidential reporting prior to publication – likely in early spring. You can find more information on the new QMs and to access the manual here.
Next steps: Access the Metrics that Matter Most
It’s of note that the next update to CMS’ Annual Payment Unit (APU) is coming in 2024 and will increase the financial penalty for noncompliance from 2% to 4%. While that may seem like plenty of time to improve your quality measures, the 2024 APU will be based on information from the CY 2022 reporting period. Thus, if you want to participate in shared savings and avoid a greater financial burden in 2024, it’s essential to understand key metrics and how you’re performing today.
Trella Health is the leader in market intelligence for the 65+ population, with extensive data sets including Medicare FFS, Medicare Advantage, commercial payers, ACOs, and DCEs. To learn more about how data insights and analytics for key metrics can help your organization control costs, improve patient outcomes, and build a stronger referral network, schedule a demo today.
- https://www.cms.gov/Medicare/Quality-Initiatives-Patient-Assessment-Instruments/Hospice-Quality-Reporting/Public-Reporting-Key-Dates-for-Providers
- https://www.cms.gov/files/document/2021aug31hospice-final-rule-webinar.pdf
- Webinar: HQRP October Forum, CMS, October 19, 2021.
Trella Health is the leader in market intelligence for the 65+ population, with extensive data sets including Medicare FFS, Medicare Advantage, commercial payers, ACOs, and DCEs. For more insights into how to stand out as a preferred referral partner, schedule a demo today.















